SQTS
Auteur: Louise R.A. Olde Nordkamp
Supervisor: Arthur A.M. Wilde
The short QT syndrome is a very rare syndrome characterized by an abnormally short QT interval and increased risk of ventricular fibrillation and cardiac death.
Clinical diagnosis
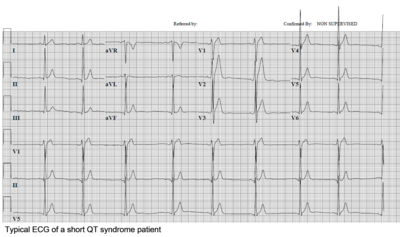
The diagnosis is based on the presence a short QT interval, in which the upper limit is mostly set on 330 ms. Males are more often affected than women. A history of cardiac arrest is present in one-third. Patients are at risk for both atrial arrhythmias (AF) and ventricular arrhythmias (VT/VF).
Physical examination
Patients can present with symptoms of arrhythmias:
- Out-of-hospital-cardiac-arrest
- Syncope, pre-syncope (weakness, lightheadedness, dizziness)
ECG tests
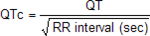
The ECG demonstrates a corrected QT interval significantly below the limit of normal (<330 ms). Additionally, notable ECG findings are the presence of a sharp T-wave beginning at the end of the QRS complex, preceded by a brief or absent ST-segment. Exercise electrocardiographic studies in SQTS patients also characteristically reveal a non-physiologic lack of QT shortening at increased heart rates.
Genetic diagnosis
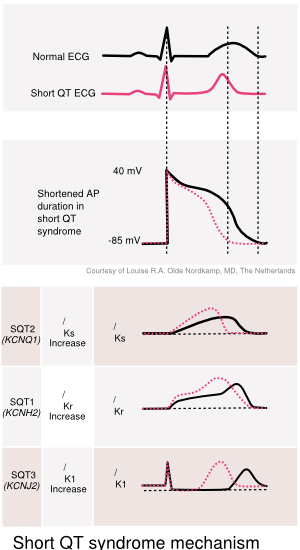
In a quarter of the patients a mutation is found, predominantly in the KCNH2 gene (SQTS1). This gain-of-function mutation causes an increase in the potassium efflux and, subsequently, to a decrease of the myocyte refractory period. Mutations in the KCNQ1, KCNJ2 and possibly CACNxxx genes are also associated with the SQTS.
Risk Stratification
Risk stratification in SQTS is still ill-defined and should be done by a specialized cardio-genetic cardiologist.
Treatment
Hydroquinidine is suggested for normalization of the QT interval in patients with a KCNH2 mutation. ICD therapy is advised in SQTS patients for secondary prevention of sudden cardiac death and could be considered
References
<biblio>
- Giustetto pmid=16926178
- Giustetto2 pmid=21798421
- Patel pmid=20716721
</biblio>