Chest Pain / Angina Pectoris
In 1772 physician William Heberden first described angina pectoris, writing: “They who are afflicted with it are seized, while they are walking (more especially if it be up hill), with a painful and most disagreeable sensation in the breast, which seems as if it would extinguish life if it were to increase or to continue, but the moment the patient stands still all this uneasiness vanishes”. REFNAME1
Stable angina (pectoris) is a clinical syndrome characterized by discomfort in the chest, jaw, shoulder, back, or arms, typically elicited by exertion or emotional stress and relieved by rest or nitroglycerin. It can be attributed to myocardial ischemia which is most commonly caused by atherosclerotic coronary artery disease.
Introduction
Three major coronary arteries supply the heart with oxygenated blood, the right coronary artery (RCA), the left anterior descending coronary artery (LAD) and the left circumflex artery (LCx). When the coronary arteries are affected by atherosclerosis and the lumen of the coronary arteries progressively narrow, a dysbalance between myocardial oxygen supply and myocardial oxygen consumption might occur, causing myocardial ischemia. This imbalance mainly occurs when oxygen demand increases due to exercise, increased heart rate, contractility or wall stress.
A complete history and physical examination are essential to support the diagnosis (stable) angina pectoris and to exclude other (acute) causes of chest pain such as an acute coronary syndrome, aortic dissection, arrhythmias, pulmonary embolism, (tension) pneumothorax or pneumonia, gastroesophageal reflux or spams, hyperventilation or musculoskeletal pain. REFNAME2 In addition, laboratory tests and specific cardiac investigations are often necessary.
History
Patients often describe angina pectoris as pressure, tightness, or heaviness located centrally in the chest, and sometimes as strangling, constricting, or burning. The pain often radiates elsewhere in the upper body, mainly arms, jaw and/or back. REFNAME3 Some patients only complain about abdominal pain so the presentation can be a specific. REFNAME4, REFNAME5
Angina pectoris however has some characteristics that can help to differentiate between other causes of (chest) pain. Angina pectoris is usually is brief and gradual in onset and offset, with the intensity increasing and decreasing over several minutes. The pain does not change with respiration or position. If patients had angina pectoris previously they are often able to recognize the pain immediately. REFNAME6
Angina pectoris usually occurs with increasing oxygen demand such as during exercise. As soon as the demand is decreased (by stopping the exercise for example) the angina pectoris usually disappears within a few minutes.
Another way to relieve pain is by administration of nitro-glycerine spray. Nitro-glycerine spray is a vasodilator which reduces venous return to the heart and therefore decreases the workload and therefore oxygen demand. It also vasodilates the coronary arteries and increases coronary blood flow. REFNAME7 The response to nitro-glycerine is however not specific for angina pectoris, a similar response may be seen with oesophageal spasm or other gastrointestinal problems because nitro-glycerine also relaxes smooth muscle. REFNAME8
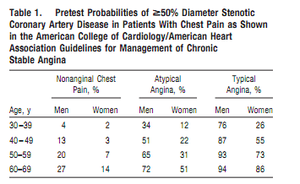
The classification of chest pain in combination with age and sex is helpful in estimating the pretest likelihood of angiographically significant coronary artery disease (Table 1).
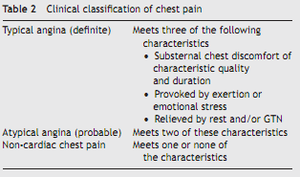
Depending on the characteristics, chest pain can be identified as typical angina, atypical angina or non-cardiac chest pain (Table 2).
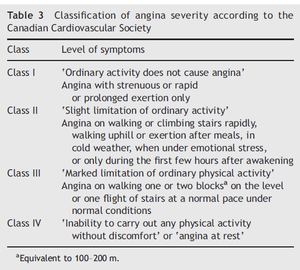
Furthermore, the intensity of the pain can be classified according to the Canadian Cardiovascular Society as shown in Table 3.
During angina pectoris so called vegetative symptoms can occur, including sweating, nausea, paleface, anxiety and agitation. This is probably caused by the autonomic nerve system being more active in a reaction to stress. REFNAME9
Finally, it is important to differentiate unstable angina (indicating an acute coronary syndrome or even myocardial infarction requiring urgent treatment) from stable angina. Unstable angina typically is severe, occurs and does not disappear with rest, and has a longer duration than stable angina. It is important to initiate the right treatment in these patients, as described in the acute coronary syndromes chapter.
Physical Examination
There are no specific signs in angina pectoris. Physical examination of a patient with (suspected) angina pectoris is important to assess the presence of hypertension, valvular heart disease, or hypertrophic obstructive cardiomyopathy. It should include the body-mass index, evidence of non-coronary vascular disease which may be asymptomatic, and other signs of co morbid conditions. Absence of palpable pulsations in the dorsal foot artery is associated with an 8 fold increase in coronary artery disease.
Electrocardiogram (ECG)
The electrocardiogram (ECG) is an easy and important tool to differentiate between unstable angina (acute coronary syndrome) and stable angina. Patients with unstable angina pectoris are likely to show abnormalities on the ECG at rest, in particular ST-segment deviations. Although a resting ECG may show signs of coronary artery disease such as pathological Q-waves indicating a previous MI or other abnormalities, most patients with stable angina pectoris often have a completely normal ECG at rest. Therefore exercise ECG testing might be necessary to show signs of myocardial ischemia. REFNAME10
Exercise ECG testing is performed with gradually increasing intensity on a treadmill or a bicycle ergo meter. Exercise increases the oxygen demand of the heart, potentially revealing myocardial ischemia by the occurrence of ST-segment depression on the ECG. REFNAME11
Laboratory Testing
Laboratory testing in the setting of angina pectoris can be useful to differentiate between different causes of the pain, including an acute coronary syndrome. Moreover, it might assist in establishing a cardiovascular risk profile.
Stress Testing in Combination with Imaging
Some patients might be unable to perform physical exercise. Furthermore, in patients with resting ECG abnormalities, it might be difficult to interpret the exercise ECG. Finally, if the ECG made during exercise testing does not show any abnormalities angina pectoris becomes very unlikely. However, if the diagnosis is still in doubt, the following additional research may be performed.
- Exercise echocardiography means that an echocardiography is made before and during different stages up to peak exercise in order to identify wall motion abnormalities. REFNAME12 An alternative is pharmacological stress testing using dobutamine.
- Myocardium Perfusion Scintigraphy (MPS) is able to show the perfusion of the heart during exercise and at rest based on radiopharmaceutical tracer uptake. REFNAME13
- Magnetic Resonance Imaging can be done with vasodilatory adenosine or stimulating dobutamine to detect wall motion abnormalities induced by ischemia during pharmacological stress. REFNAME14
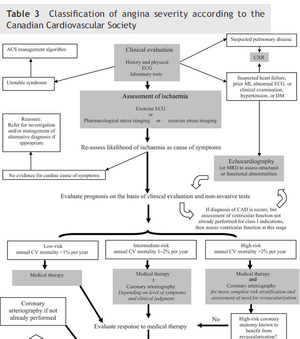
The findings on stress testing can be used to determine the choice between medical therapy only or medical therapy and invasive assessment of the coronary anatomy in patients with stable angina. Coronary angiography is recommended based upon the severity of symptoms, likelihood of ischemic disease, and risk of the patient for subsequent mortality based on stable angina pectoris risk scores. REFNAME15 For the algorithm for the initial evaluation of patients with clinical symptoms of angina (Figure 1).
Coronary Angiography (CAG)
Coronary angiography (CAG) can assist in the diagnosis and the identification of treatment options for stable angina pectoris. During CAG, the coronary anatomy is visualized including the presence of coronary luminal stenoses. A catheter is inserted into the femoral artery or into the radial artery. The tip of the catheter is positioned at the beginning of the coronary arteries and contrast fluid is injected. The contrast is made visible by X-ray and the images that are obtained are called angiograms.
If stenoses are visible, the operator will judge whether this stenosis is significant and eligible for percutaneous coronary intervention (PCI) or coronary artery bypass grafting (CABG). Ideally PCI happens immediately following the CAG but not all hospitals are entitled to carry out revascularization procedures.
Treatment
Stable angina pectoris can be treated by revascularization (PCI or CABG) or optimal medical therapy. The choice depends on factors such as the severity of symptoms and anatomical complexity of the lesion. Current guidelines for myocardial revascularization, recommend revascularization in patients with persistent symptoms despite optimal medical therapy. REFNAME16 Furthermore, revascularization is indicated in case of proven large areas of myocardial ischemia, such as a left main stem stenosis, a proximal LAD stenosis or significant three vessel disease. The choice between PCI and CABG depends on the multitude of factors, and the choice should be made in a team including (interventional) cardiologists and thoracic surgeons.
Medical Therapy
Initial treatment of stable angina pectoris focuses on medication to keep the oxygen demand of the heart as low as possible. β blockers lower heart rate and blood pressure, decreasing the oxygen demand of the heart. REFNAME17 Nitrates dilatate the coronary arteries so the heart receives more oxygenated blood. REFNAME18 Antiplatelet therapy (aspirin) reduces the risk of development of a thrombus and thus subsequent (coronary) ischemic events. REFNAME19 Apart from starting medication the patient needs to minimize/control any present risk factors like smoking, overweight and drinking alcohol. See chronic coronary diseases.
PCI
The procedure of PCI is similar to a CAG, except this time a catheter with an inflatable balloon will be brought at the site of the stenosis. Inflation of the balloon within the coronary artery will crush the atherosclerosis and eliminate the stenosis. To prevent the collapsing of the arteric wall and restenosis, a stent is often positioned at the site of the stenosis.
CABG
There are circumstances in which CABG should be considered, including left main or proximal LAD stenosis or multiple vessel disease. The choice for PCI or CABG depends on multiple patient and lesion characteristics and should be discussed in a specialized heart team involving cardiologists and cardiothoracic surgeons. With CABG, a bypass is placed around the stenosis using the internal thoracic arteries or the saphenous veins from the legs. The bypass originates proximal from the stenosis and terminates distally from the stenosis.
References
<biblio>
- REFNAME1 pmid=11756201
- REFNAME2 pmid=4997794
- REFNAME3 pmid=10099685
- REFNAME4 pmid=10866870
- REFNAME5 pmid=10751787
- REFNAME6 pmid=6831781
- REFNAME7 pmid=3925741
- REFNAME8 pmid=14678917
- REFNAME9 pmid=15289388
- REFNAME10 pmid=8375424
- REFNAME11 pmid=17162834
- REFNAME12 pmid=1352191
- REFNAME13 pmid=2007701
- REFNAME14 pmid=12566362
- REFNAME15 pmid=18061078
- REFNAME16 pmid=20802248
- REFNAME17 pmid=16735367
- REFNAME18 pmid=3925741
- REFNAME19 pmid=9355934
</biblio>