Chest Pain / Angina Pectoris
In 1772 doctor William Heberden first described angina pectoris, he wrote: “They who are afflicted with it are seized, while they are walking (more especially if it be up hill), with a painful and most disagreeable sensation in the breast, which seems as if it would extinguish life if it were to increase or to continue, but the moment the patient stands still all this uneasiness vanishes”.[1]
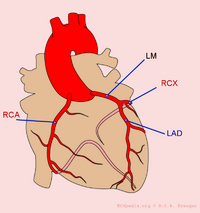
Three major coronary arteries provide the heart with oxygenated blood, the right coronary artery (RCA), the left coronary artery (LCA) and the circumflex artery (Cx). When the coronary arteries are affected by atherosclerosis and the lumen of the coronary arteries narrows, the heart receives less oxygenated blood and becomes hypoxic, which results in angina pectoris.
Complete history and physical examination are essential to determine angina pectoris as diagnosis and to exclude other causes of chest pain, such as aorta dissection, arrhythmias, pulmonary embolism, pneumonia, heartburn, hyperventilation or musculoskeletal problems.[2]
History
Patients often experience angina pectoris as if a elephant stands on their chest. Because the heart itself has very few nerves the pain can be sensible elsewhere in the upper body, mainly arms, jaw and/or back.[3] Some patients only complain about stomach ache so the presentation can be very a specific.[4],[5]
Angina pectoris however has some characteristics that can help to differentiate between other causes of (chest) pain. Angina pectoris is gradual in onset and offset, with the intensity increasing and decreasing over several minutes. The pain is constant and does not change with respiration or position. If patients had angina pectoris before they will recognize the pain immediately.[6]
Angina pectoris usually occurs during exercise when the demand for oxygenated blood increases. Coronary arteries with a narrowed lumen can not meet the demand of oxygenated blood during exercise. As soon as the exercise is aborted angina pectoris decreases. This is called stable angina pectoris.
Unstable angina pectoris means angina pectoris at rest which consists less than two months. Over time the angina pectoris develops to more often, severe and prolonged, so that symptoms are to occur at less and less effort than before.[7]
Stable angina pectoris responds to nitro-glycerine spray, unstable angina pectoris does not. Nitro-glycerine spray is a venodilator which reduces venous return to the heart and therefore decreases the workload and therefore oxygen demand. It also vasodilates the coronary arteries and increases coronary blood flow.[8]
Nitro-glycerine is however not specific for angina pectoris, a similar response may be seen with oesophageal spasm or other gastrointestinal problems because nitro-glycerine also relaxes smooth muscle.[9]
During angina pectoris so called vegetative symptoms can occur, this includes sweating, nausea, paleface, anxiety and agitation. The idea is that the vegetative nerve system is more active in a reaction to stress.[10]
Physical Examination
Oxygen deficiency of the heart leads to ischemia, ischemia and the discomfort the patient experiences lead to sympathetic activation of the nervous system. This is detectable during physical examination by an increase in heart rate and elevation in blood pressure. Ischemia can also cause a temporarily impairment in myocardial function, on auscultation you could hear a paradoxically split second heart sound, a third or fourth heart sound and a mitral regurgitation murmur. All these findings however disappear with resolution of the ischemia. Up to date: Pathophysiology and clinical presentation of ischemic chest pain, geen bronvermelding.
ECG
The electrocardiogram (ECG) is an easy and important tool to differentiate between myocardial ischemia and infarction. Patients with unstable angina pectoris will show abnormalities on the ECG at rest, in particular ST depression. Patients with stable angina pectoris are likely to have a completely normal ECG at rest, exercise ECG testing will be necessary to show any abnormalities.[11] During exercise ECG testing an ECG is made during cycling on a home trainer or walking on a treadmill. While exercising the oxygen demand of the heart increases, if the narrowed coronary arteries are unable to supply enough oxygenated blood, the patient develops pain on the chest and the ECG will show abnormalities.[12]
Additional Research
If the ECG made during exercise testing does not show any abnormalities angina pectoris becomes very unlikely. If the ECG does show abnormalities during exercise testing additional research needs to be done.[12] Depending on the hospital one of the below standing research will be done.
- Exercise echocardiography means that an echocardiography is made directly after exercise. The poorly perfused parts of the heart will show less activity.[13]
- Myocardium Perfusion Scintigraphy (MPS) is able to show the perfusion of the heart during exercise and at rest.[14]
- MRI can be done with vasodilatory dobutamine or stimulating adenosine to assess how the heart behaves during exercise.[15]
The findings on stress testing can be used to determine the choice between medical therapy and revascularization in patients with stable angina. Coronary angiography is recommended based upon symptoms, left ventricular function, and estimated risk by stress testing.[16]
Table 1
Coronary Angiography
In patients with unstable angina pectoris early coronary angiography possibly followed by revascularization is usually performed within 4 to 24 hours of admission in the hospital. In most clinical trials this strategy has shown a reduction in the incidence of death or nonfatal myocardial infraction.[7]
A CAG is an X ray examination of the coronary arteries, a catheter is inserted into the femoral artery or into the radial artery. The tip of the catheter is positioned at the beginning of the coronary arteries and contrast fluid is injected. Contrast is visible by X ray and the images that are obtained are called angiograms.
On an angiogram stenoses will be visible, if the stenosis is significant coronary intervention will take place. Ideally this happens immediately following the CAG but not all hospitals that are entitled to carry out CAG are qualified to perform percutaneous coronary intervention (PCI).
Treatment
Medication
In patients with stable angina pectoris percutaneous coronary intervention does not offer any benefit in terms of death, myocardial infarction, or the need for subsequent revascularization compared with conservative medical treatment.[17]
Initial treatment of stable angina pectoris therefore focuses on medication to keep the workload of the heart as low as possible. β blockers lower heart rate and blood pressure, this decreases the oxygen demand of the heart.[18] Nitrates dilatate the coronary arteries so the heart receives more oxygenated blood.[8] Anticoagulants (aspirin) to reduce the risk of development of a thrombus in the coronary arteries.[19]
Apart from starting medication the patient needs to minimize any present risk factors like smoking, overweight and drinking alcohol. See chronic coronary diseases.
Percutaneous Coronary Intervention
The procedure of PCI is similar to a CAG, except this time a catheter with an inflatable balloon will be brought at the site of the stenosis. Inflation of the balloon within the coronary artery will crush the atherosclerosis and eliminate the stenosis. To prevent that the effect of the balloon is only temporarily a stent is often positioned at the site of the stenosis.
Coronary Artery Bypass Graft
There are circumstances in which CABG should be performed. CABG does not eliminate the stenosis like PCI does. Using the internal thoracic arteries or the saphenous veins from the legs a bypass is made around the stenosis. The bypass originates from the aorta and terminates directly after the stenosis. Thereby restoring the blood supply to the ramifications.
Myocardial Infarction
In 2006 425.425 people died from a heart attack, 1.255.000 new and recurrent coronary attacks took place, about 34% died, 17.600.000 victims of angina, heart attack and other forms of coronary heart disease are still living.
These numbers only account for the United States.
Pathofysiology
A heart attack or myocardial infarction (MI) is an acute presentation of a process that has been going on much longer. The process responsible is atherosclerosis. Atherosclerosis is a chronic disease of the arteries in which artery walls thicken by deposition of fatty materials such as cholesterol. The result over decades are plaques, which can narrow the lumen of the arteries significantly and progressively causing symptoms as angina pectoris. Plaques can also suddenly rupture, trigger a cascade which results in a thrombus and thereby cause myocardial infarction.[20]
History
Classic presentation of a myocardial infarction is acute chest pain which lasts longer than a few minutes.[21] The pain does not decrease at rest and is only temporarily relieved with nitroglycerin. Common accompanying symptoms are radiating pain to shoulder, arm, back and/or jaw.[3] Shortness of breath can occur, as well as sweating, fainting, nausea and vomiting, so called vegetative symptoms. Some patients not really complain about chest pain but more about abdominal pain so as with angina pectoris the presentation can be very a specific.[4],[5]
It is important to complete the history with information about past history (prior history of ischemic events or vascular disease), risk factors for cardiovascular disease (o.a. smoking, hypertension, hyperlipidemia, obesity) and family history (direct family with myocardial infarction and/or sudden cardiac death).
Signs of heart failure such as orthopnea (not able to sleep without a pillow), progressive dyspnoea and oedematous ankles are indicative for the extent of the problem.[10]
A suspected myocardial infarction should be rapidly evaluated to initiate appropriate therapy.
Physical Examination
On physical examination evidence of systemic hypoperfusion can be found such as hypotension, tachycardia, impaired cognition, pale and ashen skin.[10]
If during auscultation pulmonary crackles are heard and pitting oedema of the ankles is seen heart failure is complicating the myocardial infarction.
History and physical examination are helpful to determine myocardial infarction as diagnosis and to exclude other causes of chest pain, such as angina pectoris, aorta dissection, arrhythmias, pulmonary embolism, pneumonia, heartburn, hyperventilation or musculoskeletal problems.[10]
Electrocardiogram
An electrocardiogram (ECG) should be made within 10 minutes of arrival in every patient with suspected myocardial infarction.[10] An ECG is important to differentiate between myocardial ischemia and infarction:
- ST elevation in myocardial infarction
- ST depression in myocardial ischemia
And to differentiate between STEMI and NSTEMI:
- STEMI stands for ST elevated (>20 min) Myocardial Infarction
- NSTEMI stand for Non ST elevated Myocardial Infarction
It can however take 90 minutes after the onset of the symptoms to see abnormalities on the ECG. Therefore it is important to make a serial ECG, certainly if a patient has ongoing symptoms.[10]
An ECG is also helpful in localising the ischemia: Anterior wall ischemia - One or more of leads V1-V6 Anteroseptal ischemia - Leads V1 to V3 Apical or lateral ischemia - Leads aVL and I, and leads V4 to V6 Inferior wall ischemia - Leads II, III, and aVF
Cardiac Markers
Cardiac markers are essential for confirming the diagnosis of infarction. Elevated CK MB and Troponin I indicate damage of the myocardium. Cardiac Troponin I concentration begins to rise two to three hours after myocardial ischemia.[22] It can take 4-6 hours before the CK MB concentration is elevated. The advise is to repeat the measurements after 4-6 hours.[23] A pitfall concerning elevated Troponin I can be patients with renal failure or pulmonary embolism.[24] Although cardiac markers are helpful for confirming the diagnosis reperfusion should not always wait till the cardiac markers are known.
ST elevated Myocardial Infarct
Initial treatment of STEMI is relief of ischemic pain, stabilize the hemodynamic status and reduce the ischemia as quickly as possible by fibrinolysis or primary percutaneous coronary intervention (PCI). Meanwhile other measures as continuous cardiac monitoring, oxygen and intravenous access are necessary to guarantee the safety of the patient.[10]
Rapid revascularisation is essential to minimize the impact of the myocardial infarction and thereby reduce mortality. In the first hours after symptom onset the amount of salvageable myocardium by reperfusion is greatest. [25], [26] Revascularisation can be achieved by fibrinolysis or PCI.
PCI is, if available, the preferred revascularisation method for patients with STEMI. But not all hospitals are qualified to perform PCI and therefore fibrinolysis is still used. There are however some circumstances in which transfer to a PCI qualified hospital is essential:
- Patients with contraindications for fibrinolysis as active bleedings, recent dental surgery, past history of intracranial bleeding.[27]
- Patients with cardiogenic shock, severe heart failure and/or pulmonary oedema complicating the myocardial infarction.[28], [29]
Or when PCI has a better outcome:
- Patients who present three hours to four hours after the onset of the symptoms.[30]
- Patients with a non diagnostic ECG or a atypical history a coronary angiography with the ability to perform a PCI is preferred.[30]
Fibrinolysis
Fibrinolytics like streptokinase stimulate the conversion of plasminogen to plasmin. Plasmin demolishes fibrin which is an important constituent of the thrombus. Fibrinolytics are most effective the first hours after the onset of symptoms, after twelve hours the outcome will not improve.[26] Because re occlusion after fibrinolysis is possible patients should be transferred to a PCI qualified hospital once fibrinolysis is done.[31]
Percutaneous Coronary Intervention (PCI)
Table 3 Considerations for selecting primary percutaneous coronary intervention (PCI) for reperfusion therapy in patients with ST elevation myocardial infarction (STEMI)
The procedure of PCI starts off as a coronary angiography (see CAG). When the stenosis is visualized a catheter with an inflatable balloon will be brought at the site of the stenosis. Inflation of the balloon within the coronary artery will crush the atherosclerosis and eliminate the stenosis. To prevent that the effect of the balloon is only temporarily a stent is positioned at the site of the stenosis. To reduce the risk of coronary artery stent thrombosis antiplatelet therapy should be given.
Coronary Artery Bypass Graft
There are circumstances in which CABG should be performed.
| Class of recommendations | ACC / AHA 2004 Guideline on CABG in STEMI patients [32] |
|---|---|
| Class I | There is evidence and/or general agreement that CABG should be performed in patients with STEMI in the following settings:
If possible, an internal mammary artery graft should be used to bypass a significantly stenosed left anterior descending artery. |
| Class IIa | The weight of evidence or opinion is in favor of benefit from CABG in patients with STEMI in the following settings:
|
| Class IIb | |
| Class III |
There is evidence and/or general agreement that emergency CABG should not be performed in patients with STEMI in the following settings:
|
|
Class I: Evidence and/or general agreement that a given treatment or procedure is beneficial, useful, effective. Class II: Conflicting evidence and/or a divergence of opinion about the usefulness/efficacy of the given treatment or procedure. IIa: Weight of evidence/opinion is in favour of usefulness/efficacy. IIb: Usefulness/efficacy is less well established by evidence/opinion. Class III: Evidence or general agreement that the given treatment or procedure is not usefull effective, and in some cases may be harmful. | |
CABG does not eliminate the stenosis like PCI does. Using the internal thoracic arteries or the saphenous veins from the legs a bypass is made around the stenosis. The bypass originates from the aorta and terminates directly after the stenosis. Thereby restoring the blood supply to the ramifications. A bypass can be single or multiple, multiple meaning that there are several coronary arteries bypassed using the same bypass.
Major surgery is not preferable in patients with STEMI, but CABG is inevitable when fibrinolysis and/or PCI failed or when the patient develops cardiogenic shock, life threatening ventricular arrhymthmias or three vessel disease.[33]
MEDICATION TO START AFTER MI[34] β blockers lower heart rate and blood pressure, this decreases the oxygen demand of the heart. Nitrates dilatate the coronary arteries so the heart receives more oxygenated blood. Anticoagulants reduce the risk of development of a thrombus in the coronary arteries. Statins to lower cholesterol.
Apart from starting medication the patient needs to minimize any present risk factors like smoking, overweight and drinking alcohol.
Non ST elevated Myocardial Infarct
Initial treatment in NSTEMI is to reduce ischemia, stabilize the hemodynamic status, make serial ECG and to repeat measurements of the cardiac markers. Depending on the early risk stratification a choice has to be made between early invasive therapy or conservative therapy with medicines.[10]
Early risk stratification is helpful to identify patients at high risk who need a more aggressive therapeutic approach to prevent further ischemic events.[35]
- Age ≥65 years
- Presence of at least three risk factors for coronary heart disease (hypertension, diabetes, dyslipidemia, smoking, or positive family history of early MI)
- Prior coronary stenosis of ≥50 percent
- Presence of ST segment deviation on admission ECG
- At least two anginal episodes in prior 24 hours
- Elevated serum cardiac biomarkers
- Use of aspirin in the prior seven days
Patients with a score of 0 to 1 are at low risk, score 2 to 3 are at intermediate risk, score 4 to 6 are at high risk.
Conservative Therapy
The main objective of in hospital conservative therapy is to relieve ischemic pain by intensifying medical therapy with aspirin and clopidogrel orally and nitro-glycerine, heparin and a beta blocker intravenously. If the patients becomes asymptomatic on these medication and is still asymptomatic when the medication is stopped, rest and stress imaging testing will be performed. The advantage of conservative therapy is reduction of the number of unnecessary revascularizations. The disadvantage is a prolonged stay in the hospital. Up to date: Trials of conservative versus early invasive therapy in unstable angina and non-ST elevation myocardial infarction, geen specifiekere bronvermelding.
Rest and Stress Imaging Tests
Rest and stress testing is indicated in patients with:[36]
- Angina pectoris with ECG abnormalities during exercise ECG testing
- Asymptomatic NSTEMI after in hospital conservative therapy
Exercise echocardiography means that an echocardiography is made directly after exercise. The poorly perfused parts of the heart will show less activity.[13] Myocardium Perfusion Scintigraphy (MPS) is able to show the perfusion of the heart during exercise and at rest.[14] MRI can be done with vasodilatory dobutamine or stimulating adenosine to assess how the heart behaves during exercise.[15]
Invasive Therapy
High risk patients, patients with persistent symptoms despite medication or a positive stress test need invasive therapy. Depending on what is seen during coronary angiography PCI or a CABG is indicated. (see PCI/CABG) Fibrinolytic therapy is not used in NSTEMI.[37]
Chronic Coronary Disease
Even though chronic coronary disease mortality rates have declined since 1970 it is still the leading cause of death in many western countries and in an increasing number of non western countries.[38]
The cause of the reduction in mortality rates is mainly due to rapid recognition at special cardiac care units and the possibility of early intervention.[39], [40]
But because survivors of a myocardial infarction still face a substantial risk of further cardiovascular events recognizing and reducing of risk factors is very important.
The following risk factors for chronic coronary disease are modifiable and should be tackled.[41]
Cigarette smoking damages the endothelium of the blood vessels making it easy for the cholesterol to adhere. Smoking is therefore a leading preventable cause of coronary disease. All patients who smoke should be counselled to give up smoking. Nicotine replacement therapy and behavioural therapy can help.
Hypertension is like smoking disadvantageous for the endothelium of the blood vessels and so hypertension contributes to the progression of atherosclerosis. Hypertension is defined as a systolic pressure >140 mmHg and/or diastolic pressure >90 mmHg. Patients with hypertension should be first treated with non pharmacologic therapies, including salt restriction, weight reduction in overweight/obese patients, and avoidance of excess alcohol intake. Antihypertensive drugs are indicated in patients with persistent hypertension despite non pharmacologic therapy. Most patients will require multiple antihypertensive drug therapies. Cholesterol is the felon in the atherosclerosis tale and therefore cholesterol levels in the blood should be optimal, meaning low LDL levels and high HDL levels. This can be achieved by using statins. Exercise lowers morbidity and mortality from coronary disease. Obesity increases several risk factors for coronary heart disease, including hypertension, high cholesterol and insulin resistance as well as diabetes. Data show a linear relationship of higher body weight with morbidity and mortality from coronary disease. All patients who are willing, ready and able to lose weight should receive information about behaviour modification, diet, and increased physical activity. A healthy diet results in a significantly lower risk of coronary disease. A healthy diet consists of high intake of fruit and vegetables, high fiber intake, a low glycemic index and load, unsaturated fat rather than saturated fat, a limited intake of red or processed meat and intake of omega 3 fatty acids. Several studies have shown that people who have a high intake of fruit and vegetables have a reduce risk coronary disease. It is possible that this is due to specific compounds in vegetables and fruits, or because people who eat more vegetables and fruits tend to eat less meat and saturated fat.
In diabetes mellitus tight glycemic control is important to protect against many vascular complications, including coronary disease. A small amount of alcohol results in a lower risk of morbidity and mortality from coronary disease.
Screening
Because extensive coronary disease can exist with minimal or no symptoms screening for coronary disease has been suggested. Although screening results in indentifying patients at increased risk there is lack of evidence that screening actually improves outcome.[42]
References
- Davies SW. Clinical presentation and diagnosis of coronary artery disease: stable angina. Br Med Bull. 2001;59:17-27. DOI:10.1093/bmb/59.1.17 |
- Sampson JJ and Cheitlin MD. Pathophysiology and differential diagnosis of cardiac pain. Prog Cardiovasc Dis. 1971 May;13(6):507-31. DOI:10.1016/s0033-0620(71)80001-4 |
- Foreman RD. Mechanisms of cardiac pain. Annu Rev Physiol. 1999;61:143-67. DOI:10.1146/annurev.physiol.61.1.143 |
- Canto JG, Shlipak MG, Rogers WJ, Malmgren JA, Frederick PD, Lambrew CT, Ornato JP, Barron HV, and Kiefe CI. Prevalence, clinical characteristics, and mortality among patients with myocardial infarction presenting without chest pain. JAMA. 2000 Jun 28;283(24):3223-9. DOI:10.1001/jama.283.24.3223 |
- Pope JH, Ruthazer R, Beshansky JR, Griffith JL, and Selker HP. Clinical Features of Emergency Department Patients Presenting with Symptoms Suggestive of Acute Cardiac Ischemia: A Multicenter Study. J Thromb Thrombolysis. 1998 Jul;6(1):63-74. DOI:10.1023/A:1008876322599 |
- Constant J. The clinical diagnosis of nonanginal chest pain: the differentiation of angina from nonanginal chest pain by history. Clin Cardiol. 1983 Jan;6(1):11-6. DOI:10.1002/clc.4960060102 |
- Anderson JL, Adams CD, Antman EM, Bridges CR, Califf RM, Casey DE Jr, Chavey WE 2nd, Fesmire FM, Hochman JS, Levin TN, Lincoff AM, Peterson ED, Theroux P, Wenger NK, Wright RS, Smith SC Jr, Jacobs AK, Adams CD, Anderson JL, Antman EM, Halperin JL, Hunt SA, Krumholz HM, Kushner FG, Lytle BW, Nishimura R, Ornato JP, Page RL, Riegel B, American College of Cardiology, American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non-ST-Elevation Myocardial Infarction), American College of Emergency Physicians, Society for Cardiovascular Angiography and Interventions, Society of Thoracic Surgeons, American Association of Cardiovascular and Pulmonary Rehabilitation, and Society for Academic Emergency Medicine. ACC/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-Elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non-ST-Elevation Myocardial Infarction) developed in collaboration with the American College of Emergency Physicians, the Society for Cardiovascular Angiography and Interventions, and the Society of Thoracic Surgeons endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation and the Society for Academic Emergency Medicine. J Am Coll Cardiol. 2007 Aug 14;50(7):e1-e157. DOI:10.1016/j.jacc.2007.02.013 |
- Abrams J. Hemodynamic effects of nitroglycerin and long-acting nitrates. Am Heart J. 1985 Jul;110(1 Pt 2):216-24.
- Henrikson CA, Howell EE, Bush DE, Miles JS, Meininger GR, Friedlander T, Bushnell AC, and Chandra-Strobos N. Chest pain relief by nitroglycerin does not predict active coronary artery disease. Ann Intern Med. 2003 Dec 16;139(12):979-86. DOI:10.7326/0003-4819-139-12-200312160-00007 |
- Antman EM, Anbe DT, Armstrong PW, Bates ER, Green LA, Hand M, Hochman JS, Krumholz HM, Kushner FG, Lamas GA, Mullany CJ, Ornato JP, Pearle DL, Sloan MA, Smith SC Jr, Alpert JS, Anderson JL, Faxon DP, Fuster V, Gibbons RJ, Gregoratos G, Halperin JL, Hiratzka LF, Hunt SA, Jacobs AK, and American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction--executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). Circulation. 2004 Aug 3;110(5):588-636. DOI:10.1161/01.CIR.0000134791.68010.FA |
- Guidelines for cardiac exercise testing. ESC Working Group on Exercise Physiology, Physiopathology and Electrocardiography. Eur Heart J. 1993 Jul;14(7):969-88.
- Fox K, García MA, Ardissino D, Buszman P, Camici PG, Crea F, Daly C, de Backer G, Hjemdahl P, López-Sendón J, Morais J, Pepper J, Sechtem U, Simoons M, Thygesen K, and Grupo de trabajo de la sociedad europea de cardiologia sobre el manejo de la angina estable. [Guidelines on the management of stable angina pectoris. Executive summary]. Rev Esp Cardiol. 2006 Sep;59(9):919-70. DOI:10.1157/13092800 |
- Amanullah AM and Lindvall K. Predischarge exercise echocardiography in patients with unstable angina who respond to medical treatment. Clin Cardiol. 1992 Jun;15(6):417-23. DOI:10.1002/clc.4960150605 |
- Brown KA. Prognostic value of thallium-201 myocardial perfusion imaging in patients with unstable angina who respond to medical treatment. J Am Coll Cardiol. 1991 Apr;17(5):1053-7. DOI:10.1016/0735-1097(91)90829-x |
- Kwong RY, Schussheim AE, Rekhraj S, Aletras AH, Geller N, Davis J, Christian TF, Balaban RS, and Arai AE. Detecting acute coronary syndrome in the emergency department with cardiac magnetic resonance imaging. Circulation. 2003 Feb 4;107(4):531-7. DOI:10.1161/01.cir.0000047527.11221.29 |
- Fraker TD Jr, Fihn SD, 2002 Chronic Stable Angina Writing Committee, American College of Cardiology, American Heart Association, Gibbons RJ, Abrams J, Chatterjee K, Daley J, Deedwania PC, Douglas JS, Ferguson TB Jr, Gardin JM, O'Rourke RA, Williams SV, Smith SC Jr, Jacobs AK, Adams CD, Anderson JL, Buller CE, Creager MA, Ettinger SM, Halperin JL, Hunt SA, Krumholz HM, Kushner FG, Lytle BW, Nishimura R, Page RL, Riegel B, Tarkington LG, and Yancy CW. 2007 chronic angina focused update of the ACC/AHA 2002 guidelines for the management of patients with chronic stable angina: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines Writing Group to develop the focused update of the 2002 guidelines for the management of patients with chronic stable angina. J Am Coll Cardiol. 2007 Dec 4;50(23):2264-74. DOI:10.1016/j.jacc.2007.08.002 |
- Katritsis DG and Ioannidis JP. Percutaneous coronary intervention versus conservative therapy in nonacute coronary artery disease: a meta-analysis. Circulation. 2005 Jun 7;111(22):2906-12. DOI:10.1161/CIRCULATIONAHA.104.521864 |
- Fox K, Garcia MA, Ardissino D, Buszman P, Camici PG, Crea F, Daly C, De Backer G, Hjemdahl P, Lopez-Sendon J, Marco J, Morais J, Pepper J, Sechtem U, Simoons M, Thygesen K, Priori SG, Blanc JJ, Budaj A, Camm J, Dean V, Deckers J, Dickstein K, Lekakis J, McGregor K, Metra M, Morais J, Osterspey A, Tamargo J, Zamorano JL, Task Force on the Management of Stable Angina Pectoris of the European Society of Cardiology, and ESC Committee for Practice Guidelines (CPG). Guidelines on the management of stable angina pectoris: executive summary: The Task Force on the Management of Stable Angina Pectoris of the European Society of Cardiology. Eur Heart J. 2006 Jun;27(11):1341-81. DOI:10.1093/eurheartj/ehl001 |
- Hennekens CH, Dyken ML, and Fuster V. Aspirin as a therapeutic agent in cardiovascular disease: a statement for healthcare professionals from the American Heart Association. Circulation. 1997 Oct 21;96(8):2751-3. DOI:10.1161/01.cir.96.8.2751 |
- Davies MJ. Pathophysiology of acute coronary syndromes. Indian Heart J. 2000 Jul-Aug;52(4):473-9.
- Swap CJ and Nagurney JT. Value and limitations of chest pain history in the evaluation of patients with suspected acute coronary syndromes. JAMA. 2005 Nov 23;294(20):2623-9. DOI:10.1001/jama.294.20.2623 |
- Macrae AR, Kavsak PA, Lustig V, Bhargava R, Vandersluis R, Palomaki GE, Yerna MJ, and Jaffe AS. Assessing the requirement for the 6-hour interval between specimens in the American Heart Association Classification of Myocardial Infarction in Epidemiology and Clinical Research Studies. Clin Chem. 2006 May;52(5):812-8. DOI:10.1373/clinchem.2005.059550 |
- Puleo PR, Meyer D, Wathen C, Tawa CB, Wheeler S, Hamburg RJ, Ali N, Obermueller SD, Triana JF, and Zimmerman JL. Use of a rapid assay of subforms of creatine kinase MB to diagnose or rule out acute myocardial infarction. N Engl J Med. 1994 Sep 1;331(9):561-6. DOI:10.1056/NEJM199409013310901 |
- Thygesen K, Alpert JS, White HD, Joint ESC/ACCF/AHA/WHF Task Force for the Redefinition of Myocardial Infarction, Jaffe AS, Apple FS, Galvani M, Katus HA, Newby LK, Ravkilde J, Chaitman B, Clemmensen PM, Dellborg M, Hod H, Porela P, Underwood R, Bax JJ, Beller GA, Bonow R, Van der Wall EE, Bassand JP, Wijns W, Ferguson TB, Steg PG, Uretsky BF, Williams DO, Armstrong PW, Antman EM, Fox KA, Hamm CW, Ohman EM, Simoons ML, Poole-Wilson PA, Gurfinkel EP, Lopez-Sendon JL, Pais P, Mendis S, Zhu JR, Wallentin LC, Fernández-Avilés F, Fox KM, Parkhomenko AN, Priori SG, Tendera M, Voipio-Pulkki LM, Vahanian A, Camm AJ, De Caterina R, Dean V, Dickstein K, Filippatos G, Funck-Brentano C, Hellemans I, Kristensen SD, McGregor K, Sechtem U, Silber S, Tendera M, Widimsky P, Zamorano JL, Morais J, Brener S, Harrington R, Morrow D, Lim M, Martinez-Rios MA, Steinhubl S, Levine GN, Gibler WB, Goff D, Tubaro M, Dudek D, and Al-Attar N. Universal definition of myocardial infarction. Circulation. 2007 Nov 27;116(22):2634-53. DOI:10.1161/CIRCULATIONAHA.107.187397 |
- Anderson JL, Karagounis LA, and Califf RM. Metaanalysis of five reported studies on the relation of early coronary patency grades with mortality and outcomes after acute myocardial infarction. Am J Cardiol. 1996 Jul 1;78(1):1-8. DOI:10.1016/s0002-9149(96)00217-2 |
- Bassand JP, Danchin N, Filippatos G, Gitt A, Hamm C, Silber S, Tubaro M, and Weidinger F. Implementation of reperfusion therapy in acute myocardial infarction. A policy statement from the European Society of Cardiology. Eur Heart J. 2005 Dec;26(24):2733-41. DOI:10.1093/eurheartj/ehi673 |
- Grzybowski M, Clements EA, Parsons L, Welch R, Tintinalli AT, Ross MA, and Zalenski RJ. Mortality benefit of immediate revascularization of acute ST-segment elevation myocardial infarction in patients with contraindications to thrombolytic therapy: a propensity analysis. JAMA. 2003 Oct 8;290(14):1891-8. DOI:10.1001/jama.290.14.1891 |
- Thune JJ, Hoefsten DE, Lindholm MG, Mortensen LS, Andersen HR, Nielsen TT, Kober L, Kelbaek H, and Danish Multicenter Randomized Study on Fibrinolytic Therapy Versus Acute Coronary Angioplasty in Acute Myocardial Infarction (DANAMI)-2 Investigators. Simple risk stratification at admission to identify patients with reduced mortality from primary angioplasty. Circulation. 2005 Sep 27;112(13):2017-21. DOI:10.1161/CIRCULATIONAHA.105.558676 |
- Kent DM, Schmid CH, Lau J, and Selker HP. Is primary angioplasty for some as good as primary angioplasty for all?. J Gen Intern Med. 2002 Dec;17(12):887-94. DOI:10.1046/j.1525-1497.2002.11232.x |
- Van de Werf F, Ardissino D, Betriu A, Cokkinos DV, Falk E, Fox KA, Julian D, Lengyel M, Neumann FJ, Ruzyllo W, Thygesen C, Underwood SR, Vahanian A, Verheugt FW, Wijns W, and Task Force on the Management of Acute Myocardial Infarction of the European Society of Cardiology. Management of acute myocardial infarction in patients presenting with ST-segment elevation. The Task Force on the Management of Acute Myocardial Infarction of the European Society of Cardiology. Eur Heart J. 2003 Jan;24(1):28-66. DOI:10.1016/s0195-668x(02)00618-8 |
-
pmid=f15769784
- Eagle KA, Guyton RA, Davidoff R, Edwards FH, Ewy GA, Gardner TJ, Hart JC, Herrmann HC, Hillis LD, Hutter AM Jr, Lytle BW, Marlow RA, Nugent WC, Orszulak TA, American College of Cardiology, and American Heart Association. ACC/AHA 2004 guideline update for coronary artery bypass graft surgery: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1999 Guidelines for Coronary Artery Bypass Graft Surgery). Circulation. 2004 Oct 5;110(14):e340-437.
- Canadian Cardiovascular Society, American Academy of Family Physicians, American College of Cardiology, American Heart Association, Antman EM, Hand M, Armstrong PW, Bates ER, Green LA, Halasyamani LK, Hochman JS, Krumholz HM, Lamas GA, Mullany CJ, Pearle DL, Sloan MA, Smith SC Jr, Anbe DT, Kushner FG, Ornato JP, Pearle DL, Sloan MA, Jacobs AK, Adams CD, Anderson JL, Buller CE, Creager MA, Ettinger SM, Halperin JL, Hunt SA, Lytle BW, Nishimura R, Page RL, Riegel B, Tarkington LG, and Yancy CW. 2007 focused update of the ACC/AHA 2004 guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2008 Jan 15;51(2):210-47. DOI:10.1016/j.jacc.2007.10.001 |
- Antman EM, Anbe DT, Armstrong PW, Bates ER, Green LA, Hand M, Hochman JS, Krumholz HM, Kushner FG, Lamas GA, Mullany CJ, Ornato JP, Pearle DL, Sloan MA, Smith SC Jr, Alpert JS, Anderson JL, Faxon DP, Fuster V, Gibbons RJ, Gregoratos G, Halperin JL, Hiratzka LF, Hunt SA, Jacobs AK, American College of Cardiology, American Heart Association Task Force on Practice Guidelines, and Canadian Cardiovascular Society. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients with Acute Myocardial Infarction). Circulation. 2004 Aug 31;110(9):e82-292.
- Antman EM, Cohen M, Bernink PJ, McCabe CH, Horacek T, Papuchis G, Mautner B, Corbalan R, Radley D, and Braunwald E. The TIMI risk score for unstable angina/non-ST elevation MI: A method for prognostication and therapeutic decision making. JAMA. 2000 Aug 16;284(7):835-42. DOI:10.1001/jama.284.7.835 |
- Klocke FJ, Baird MG, Lorell BH, Bateman TM, Messer JV, Berman DS, O'Gara PT, Carabello BA, Russell RO Jr, Cerqueira MD, St John Sutton MG, DeMaria AN, Udelson JE, Kennedy JW, Verani MS, Williams KA, Antman EM, Smith SC Jr, Alpert JS, Gregoratos G, Anderson JL, Hiratzka LF, Faxon DP, Hunt SA, Fuster V, Jacobs AK, Gibbons RJ, Russell RO, American College of Cardiology, American Heart Association Task Force on Practice Guidelines, and American Society for Nuclear Cardiology. ACC/AHA/ASNC guidelines for the clinical use of cardiac radionuclide imaging--executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (ACC/AHA/ASNC Committee to Revise the 1995 Guidelines for the Clinical Use of Cardiac Radionuclide Imaging). Circulation. 2003 Sep 16;108(11):1404-18. DOI:10.1161/01.CIR.0000080946.42225.4D |
- Effects of tissue plasminogen activator and a comparison of early invasive and conservative strategies in unstable angina and non-Q-wave myocardial infarction. Results of the TIMI IIIB Trial. Thrombolysis in Myocardial Ischemia. Circulation. 1994 Apr;89(4):1545-56. DOI:10.1161/01.cir.89.4.1545 |
- Lloyd-Jones D, Adams RJ, Brown TM, Carnethon M, Dai S, De Simone G, Ferguson TB, Ford E, Furie K, Gillespie C, Go A, Greenlund K, Haase N, Hailpern S, Ho PM, Howard V, Kissela B, Kittner S, Lackland D, Lisabeth L, Marelli A, McDermott MM, Meigs J, Mozaffarian D, Mussolino M, Nichol G, Roger VL, Rosamond W, Sacco R, Sorlie P, Stafford R, Thom T, Wasserthiel-Smoller S, Wong ND, Wylie-Rosett J, and American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Executive summary: heart disease and stroke statistics--2010 update: a report from the American Heart Association. Circulation. 2010 Feb 23;121(7):948-54. DOI:10.1161/CIRCULATIONAHA.109.192666 |
- Capewell S, Beaglehole R, Seddon M, and McMurray J. Explanation for the decline in coronary heart disease mortality rates in Auckland, New Zealand, between 1982 and 1993. Circulation. 2000 Sep 26;102(13):1511-6. DOI:10.1161/01.cir.102.13.1511 |
- Heidenreich PA and McClellan M. Trends in treatment and outcomes for acute myocardial infarction: 1975-1995. Am J Med. 2001 Feb 15;110(3):165-74. DOI:10.1016/s0002-9343(00)00712-9 |
- Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, McQueen M, Budaj A, Pais P, Varigos J, Lisheng L, and INTERHEART Study Investigators. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet. 2004 Sep 11-17;364(9438):937-52. DOI:10.1016/S0140-6736(04)17018-9 |
- Gibbons RJ, Balady GJ, Bricker JT, Chaitman BR, Fletcher GF, Froelicher VF, Mark DB, McCallister BD, Mooss AN, O'Reilly MG, Winters WL, Gibbons RJ, Antman EM, Alpert JS, Faxon DP, Fuster V, Gregoratos G, Hiratzka LF, Jacobs AK, Russell RO, Smith SC, and American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Committee to Update the 1997 Exercise Testing Guidelines. ACC/AHA 2002 guideline update for exercise testing: summary article. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). J Am Coll Cardiol. 2002 Oct 16;40(8):1531-40. DOI:10.1016/s0735-1097(02)02164-2 |